I’ve talked some before about the frustration I have around pregnancy health. With pregnancy being such a personal and health-related thing, I think a lot of discussion around complications and how we’re feeling during pregnancy is also personal, and some of it taboo. It’s pretty rare when I see pregnant people share in public about the struggles they face, and I only really learn about them when I’m forthcoming myself, or join a private group that’s specific to the topic.
I don’t like that. I feel like I’ve gone into pregnancy and motherhood so blindly because of how everyone slaps a rosey picture on it. It’s only when you peel back the layers that you get to the jokes around parenthood, and the raw truth that created those jokes. Pregnancy has been so hard for me. I don’t feel like a glowing miracle. I feel sick and tired most of the time.
So this is where I publicly talk about my gestational diabetes mellitus (GDM) diagnosis. I was diagnosed with it on September 30th, and it really threw me because it’s something I didn’t have with my first pregnancy and my only risk factors are age and weight.
Before my diagnosis, I hardly knew anything about diabetes. That means I didn’t realize what was in store for me when I was in the office with my doctor, but after some reading online and meeting with a diabetes nutritionist, I quickly learned that it’s not good. I won’t dig into the risks to the baby and myself here, but they would be significant if I didn’t get my blood sugar under control. Getting there meant a total overhaul of my diet, and taking blood sugar readings at least four times a day.
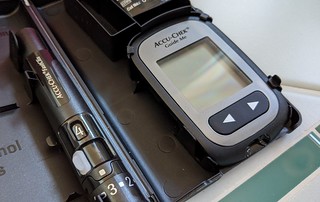
The diet overhaul included reducing my carbohydrate (including sugar) intake drastically, eating smaller meals, and making sure I eat every 2-3 hours. As someone with a busy schedule, historically carb-heavy diet, and a big comfort-eater, this has been very, very hard. And this is on top of an already difficult and painful pregnancy. The first week I started incorporating the new diet was hungry constantly and lost about five pounds, not something you want to see in the third trimester of pregnancy! Turns out I cut out too many carbs and was really bad about making sure I ate often enough, as I’m not naturally much of a snack person. So, in addition to a glucose meter and all its accessories, I now own a food scale, and have measuring cups constantly at hand to make sure I’m getting the right amount of carbs as directed by the nutritionist.
Some days are harder than others, for sure. Some mornings I still cry before pulling myself together for the day. With the severe pelvic pain I’m still dealing with, the walking exercise that the nutritionist calls “free medicine” isn’t always an option for me, and if I push through the pain anyway, I pay for it dearly. Eating on a schedule is hard too, with work meetings popping up at random hours throughout the day and my need to eat not always syncing up with when my family is eating (so lonely!). Additionally, one of the suggestions from the nutritionist was eating dinner before 7PM (we’re traditionally an 8:30PM dinner family) and then have a snack before bed to see if that helps my fasting numbers overnight. This is hard for a variety of reasons.
And it’s still not all under my control. Fasting numbers overnight are still slightly higher than the nutritionist would like to see, so there’s a high chance I’ll end up needing daily insulin injections to keep them in the safe range. I spent some time at the doctor on Wednesday getting trained on how to inject it.
Still, I’m coping with all of this the best I can, and trying to focus on the bright side. First, the results came back the day after my birthday, so I got that last bit of pizza and cake in blissful ignorance! But on a more serious note, I can handle all of this, even with the bouts of crying here and there. The finger pricks for the glucose monitoring are only scary the first few times. If I end up needing them, insulin injections aren’t as scary as I had feared. The strict diet is only for a couple months. I’m also lucky that MJ has done a keto diet in the past, so he’s familiar with carb reduction and the food choices available, and he’s been right there with me as I learned to use the glucose meter (did I mention that it needs blood?!).
It was a wake-up call though. The CDC states that 50% of people with GDM go on to develop Type 2 diabetes later in life. Having this experience has convinced me that I don’t want to be in that half. I’m fortunate that it doesn’t run in my family, so I have a good chance of getting ahead of this with diet and exercise. I know I won’t be able to adhere to the strict diet I’m on for the pregnancy, but I will take these strategies I’m learning to heart to make sure most of my diet is better than it has been in the past. Exercise will also take priority as soon as I’ve recovered from birth and the first few weeks of “we have a newborn!” exhaustion.
Otherwise, I’m having regular ultrasounds, and everything looks good, so I will also continue to be grateful for that too. Next week I start non-stress tests twice a week until birth, which I was able to schedule for late in the day so it doesn’t impact my work schedule.
My heart genuinely goes out to families who don’t have the privilege we have. Even the easiest pregnancy takes such a toll on every part of you. Adding in complications like GDM makes it exponentially harder.